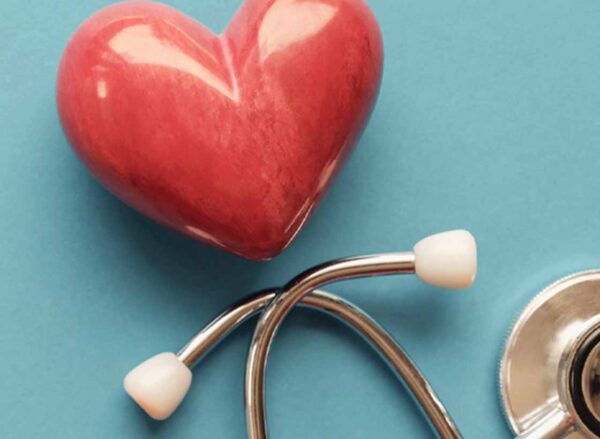
Why engagement fails
Traditional benefits engagement is broken because it’s disconnected.
- The frequency gap: Communications are episodic.
- The complexity gap: Enrollment is overwhelming—leading to “safe,” but expensive choices.
- The momentum gap: Behavior change isn’t supported after the first 30 days.
- The insight gap: Data exists, but it isn’t turned into timely, targeted action.

How we fix it
We turn engagement from episodic moments into a systematic cycle—from day-one awareness to enrollment to year-round activation.
- Clear communications drive action.
- Guided enrollment drives better plan choices.
- Personalized nudges drive better benefits utilization.
- Better choices and utilization drive measurable cost savings.

Engagement Solutions
From insight to impact: Elevating employee engagement

Who we are
bswift Engagement Solutions is our award-winning engagement strategy and custom communications team—agency-level consultants, writers, and creatives backed by 20+ years supporting complex HR and internal communications.

What we do
We start with engagement strategy and planning, then bring it to life through custom creative and activation. The result is benefits communications and digital experiences built around your plan design, channels, and workforce needs—emails, guides, landing pages, toolkits, videos, and more.

How we work
An extension of your team with strategic planning, fast execution, and continuous optimization—tailored by audience and moment. In lockstep with bswift Client Services, we align messaging to operations and key dates so communications land when they matter most.

What sets us apart
Agency-caliber strategy and creative, embedded in the bswift ecosystem. With platform context and operational insight behind every campaign, we elevate the end-to-end experience—so employees notice what matters and know what to do next.
What we offer

Benefits & HR Communications
Clear, consistent messaging for benefits, wellbeing, and HR programs.

Total Rewards Strategy
Storylines and tools that make the full rewards picture easy to grasp.

Strategic Communications & Change Management
Plans and messaging that build buy-in and reduce friction.

Leader & Manager Communications
Toolkits, talking points, and coaching so leaders can communicate with confidence.

Research & Measurement
Audits, surveys, and performance reviews that show what’s working and where to focus.

Systems Design & Process Optimization
Channel and workflow design so your comms run smoothly long into the future.
Award-winning creative and communications

Trusted by leaders who understand the stakes
Ready to deliver clearer, more impactful communications?
Get in touchEmma EnrollPro
Simplify enrollment with personalized, step-by-step guidance powered by AI-native Emma Intelligence.
Emma EnrollPro is bswift’s AI-native decision-support and enrollment guidance experience. It clarifies plan trade-offs and makes personalized recommendations using claims data, enrollment history, eligibility rules, and plan design—so employees can enroll with complete confidence.
- Increase benefits adoption
- Support smarter elections
- Improve the employee experience
- Maximize employee satisfaction

lift in voluntary benefits enrollment

reduction in enrollment time

choose Emma’s recommendation


Offers Preferred Plan Steering
When multiple plans fit, Emma EnrollPro can prioritize your preferred plan to guide utilization and support cost-control goals.

Supports Voluntary Benefits Too
Make voluntary benefits easier to understand so employees know what’s available, what it means, and are more likely to enroll.

Integrates Evive Profile Builder
Emma EnrollPro captures preferences during enrollment to personalize Evive outreach and sustain engagement year-round.
Want a demo of the Emma EnrollPro experience?
Get in touchEvive
Personalized, data-driven engagement—at scale
Evive™ extends your strategy with always-on, data-driven nudges and campaigns. Using claims data and Emma Intelligence, Evive powers measurable engagement with messaging that stays timely, relevant, and personalized to each employee’s needs and goals.
- Sustain Awareness
- Drive behaviors
- Improve habits and outcomes
- Reduce claims costs

boost in plan completions

lift in closed care gaps (year one)

average annual savings
How Evive works
Automation
Launch and manage multi-channel outreach at scale.
Personalization
Target messages by need, behavior, or eligibility.
Measurement
Track reach, frequency, and action—not just clicks.
Optimization
See what’s working and adapt in real time.

200+ campaigns, and counting
We’re constantly adding new campaigns based on client goals, population needs, and cost drivers.
- Disease Management (Cardiovascular, Cancer, Diabetes, etc)
- Mental and Behavioral Health
- Spending Accounts and Commuter Benefits
- 401(k) and Retirement Savings
- College Savings, Debt, and Tuition Support
- Family Planning Services
- Personal Finance Coaching
- Fitness, Wellness, and Health Coaching
- GLP-1 and Weight Management
- Voluntary Benefits

Evive Claims-Powered Personalization
Evive layers in medical and pharmacy claims to facilitate richer, context-aware engagement based on real employee behavior and spending. Our systems are designed with governance in mind, offering client-controlled configuration and privacy safeguards.
- Trigger nudges from actual utilization, not just eligibility
- Highlight lower-cost, higher-value options at key decision points
- Gain clearer visibility into claims cost savings and impact over time

See how Evive can power cost savings at your organization
Get in touchComplete Benefits Administration
AI-native technology, hands-on service, and decades of expertise all working together to elevate every part of your benefits experience.

COBRA, Billing & Compliance Services
Reduce risk and take the regulatory workload off your plate.
We handle dependent verification, COBRA, retirement, and payroll reconciliation—combining AI precision with human expertise, so your team can stay focused while reducing risk.
Benefits Administration Platform
Turn complexity into calm.
Handles any workforce, anywhere with deep configurability and hundreds of integrations, so complexity never slows you down. Offers maximum flexibility
and complete control.

Employee Service & Support
Resolve issues fast with self-service plus expert human care.
Employees get instant answers through Emma™ Chat and IVR, while our Service Center provides expert, empathetic support for more complex moments. It’s how we keep enrollment season calm—and surprisingly quiet.
Frequently Asked Questions

How does bswift transform employee engagement?
bswift transforms employee engagement by connecting communications, AI-guided enrollment, and year-round personalization into one continuous system. Instead of treating engagement as a seasonal event, bswift drives participation before enrollment, guides smarter decisions during enrollment, and reinforces behavior change throughout the year. The result is higher benefits participation and measurable cost impact.

What are bswift Engagement Solutions?
bswift Engagement Solutions is bswift’s in-house engagement strategy and communications team, focused on helping employers turn complex benefits programs into clear, compelling employee experiences. Working closely with bswift Client Services and the broader platform ecosystem, the team combines strategic planning, custom communications, and creative execution to build awareness, drive participation, and guide employees to take the right actions at the right time—from open enrollment campaigns to year-round engagement initiatives.

What is Evive and how does it work?
Evive™ is a capability built in to the bswift benefits platform that powers year-round personalized engagement. It uses eligibility data, enrollment history, and claims-aware insights to deliver targeted nudges and campaigns that encourage better benefits utilization. Evive helps sustain engagement beyond enrollment season and supports measurable savings through smarter usage patterns.

What is Emma EnrollPro and how does it work?
Emma EnrollPro™ is AI-guided enrollment decision support powered by Emma™ Intelligence. It analyzes plan rules, eligibility logic, prior enrollment, and claims data to clarify trade-offs and recommend the best-fit options. Employees complete enrollment faster and more confidently, improving plan alignment and voluntary benefits adoption.

What is Emma Intelligence™?
Emma™ Intelligence is bswift’s AI-native technology woven across the bswift ecosystem to make benefits simpler, smarter, and more human—reducing friction for employees, admins, and service teams. It uses benefits materials, plan configuration, eligibility logic, and operational context to guide decisions, accelerate answers, catch issues earlier, and turn data into direction.

What does AI-native mean in Emma Intelligence?
AI-native means Emma™ Intelligence is built directly into the bswift platform and workflows—not added on as a separate chatbot or bolt-on tool. Because it runs on your real benefits configuration and content, it delivers plan-specific answers and automation that match what’s actually true for each employer and employee.

How does claims data integration improve employee engagement?
Claims data enables context-aware engagement by identifying utilization patterns and potential cost drivers. When combined with eligibility and enrollment data, it allows for targeted outreach at moments that matter. This improves relevance and supports better healthcare and financial decisions.

How does personalization improve benefits utilization?
Personalization improves utilization by delivering timely, relevant messages based on individual eligibility, elections, and behavior. Instead of generic reminders, employees receive nudges aligned to their specific needs. This increases engagement and supports healthier, more cost-effective choices.

What role does continuous engagement play in benefits strategy?
Continuous engagement shifts benefits strategy from seasonal communication to year-round behavior management. By reinforcing decisions beyond enrollment, employers influence utilization, preventive care, and voluntary participation. This sustained model drives long-term outcomes and cost control.

What makes bswift’s engagement approach different from standalone engagement vendors?
Unlike standalone vendors, bswift’s engagement capabilities operate within the same ecosystem that administers benefits. Communications, enrollment guidance, and personalization all reflect real plan configuration and eligibility data. This closed-loop structure ensures that messaging, recommendations, and activation align with what is actually true for each employee.